Sports Medicine Institute
What does it take to keep top athletes on the field performing at their very best? Grab some athletic tape, have the scalpel on standby, and come find out!
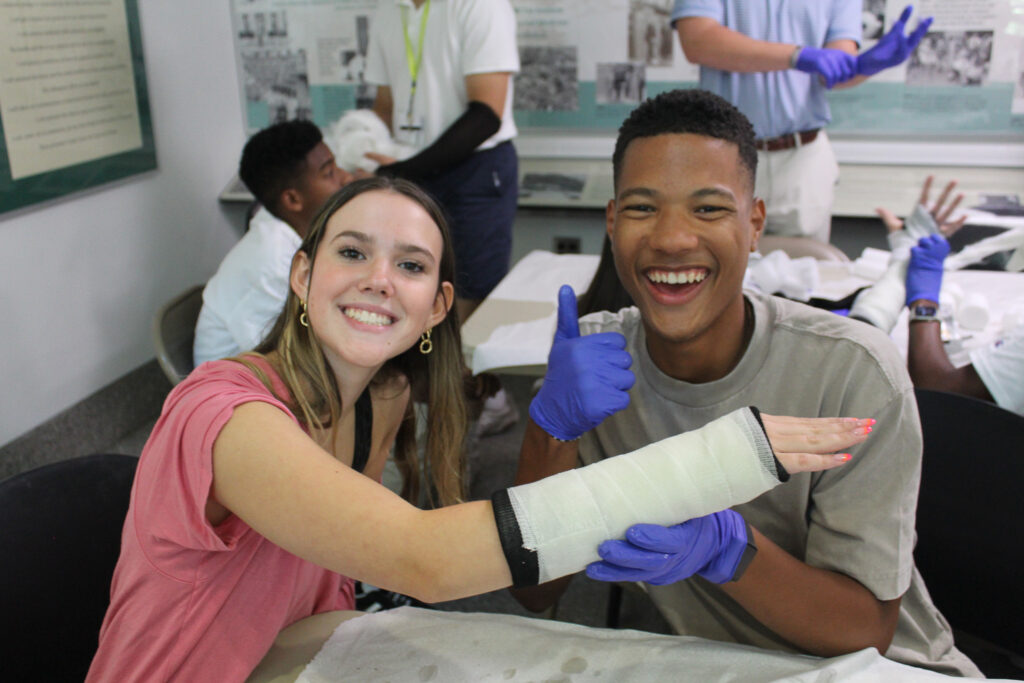
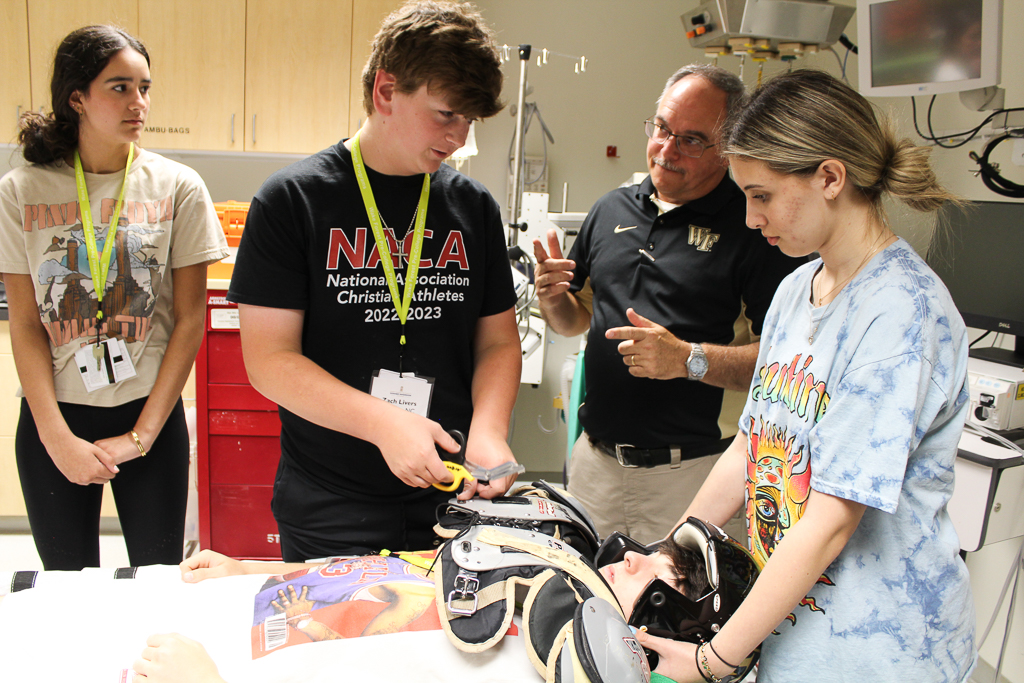
The Wake Forest Summer Immersion Sports Medicine Institute will expose students to innovative methods of medical care for the nation’s most elite athletes while exploring the various career options that the sports medicine field offers. This program will provide hands-on educational experiences emphasizing the fundamentals of sports medicine, injury prevention, rehabilitation, and athletic performance. Students will learn from esteemed Orthopaedic Sports Medicine Surgeons, Dr. Gary Poehling and Dr. Nicholas Trasolini, as well as countless experienced orthopedic surgeons, physical therapists, physician assistants, athletic trainers, and more! Some highlights of this program include a cadaveric dissection of knee and shoulder anatomy, hands-on arthroscopy experience, a casting workshop, and a visit to the world-renowned Wake Forest Pitching Lab. If you are interested in careers at the intersection of medicine and sport, this is the program for you!
At a Glance
2025 Dates: Week of June 22 – 27 (waitlist implemented) or week of July 13 – 18 (waitlist implemented)
A waitlist has been implemented for the summer 2025 Sports Medicine Institute. Students may still apply or register for different institute sessions or for the Online Immersion Program – study online with Wake Forest anywhere, anytime, at your own pace.
Program Length: Sunday – Friday, overnight
Who Can Apply?: Current 9th – 12th grade students
Tuition: $3,400
*Tuition is subject to change per year
Location: Winston-Salem, NC – Wake Forest University Reynolda Campus
*Courses carry no secondary school or college credit. Upon completion of the program, an official Wake Forest University Certificate of Completion will be awarded to all Sports Medicine Institute participants.
What You’ll Experience
Topics Covered:
- Concussions
- Athletic Training and Physical Therapy
- Knee and Shoulder Injuries
- Pediatric Sports Medicine
- Prosthetic Design, Biologics & Regenerative Medicine
Hands-On Experiences:
- Visit the WFU Pitching Biomechanics Lab and WFU Athletic Training Facilities
- Surgical Skills Labs in a Mock OR in the Hospital
- Splinting/Casting & Ankle Taping Techniques
- Suturing Lab
- Guided Cadaveric Surgical Anatomy Lab
*Hands-on experiences are subject to change.
A Day in the Life
Typical Daily Schedule
- 8:00 am – Morning Meeting and Breakfast
- 9:00 am – Welcome from Academic Leaders
- 9:30 am – Travel to Atrium Health Wake Forest Baptist Medical Center
- 10:00 am – Hands and Upper Extremity in Sports Medicine
- 12:00 pm – Lunch
- 1:00 pm – Orthopaedic Skills Labs Rotations
- 3:00 pm – Panel: Physicians Assistants Career Pathway
- 5:00 pm – Debrief of the Day
- 5:30 pm – Dinner
- 6:30 pm – Evening Activities
- 7:30 pm – Free Time
- 9:00 pm – Prepare for Bed
- 10:30 pm – Lights Out
*The “A Day in the Life” sample schedule is subject to change.

Meet the Academic Leaders

Dr. Nick Trasolini
Academic Leader, Sports Medicine Institute
Dr. Trasolini is a board-eligible, orthopaedic surgeon specializing in adult and adolescent sports medicine, arthroscopic surgery, joint perseveration, tendon and ligament injuries, shoulder and elbow injuries, cartilage and meniscus injuries, management of early arthritis, and athletic hip injuries. He has extensive training in minimally invasive arthroscopic surgery as well as complex surgeries of the knee, shoulder, elbow, and hip. Dr. Trasolini completed his residency training in Los Angeles at the University of Southern California, Keck Medical Center, and Los Angeles County Hospital where he held leadership roles as an Administrative Chief Resident. He subsequently completed fellowship training in Sports Medicine and Shoulder Surgery at Rush University Medical Center in Chicago, where he served as an assistant team physician for the Chicago White Sox (MLB), DePaul University, and the Chicago Steel (USHL). Dr. Trasolini has over 50 research publications and frequently presents at regional and national meetings. He is currently a team physician for Wake Forest University Football and local high schools. Outside of work, he enjoys spending time with his wife, Olivia, and two children Dean, and Summer.

Dr. Gary Poehling
Academic Leader, Sports Medicine Institute
Dr. Gary Poehling was born and raised in LaCrosse, Wisconsin. He received his Bachelor’s degree in Biology from Marquette University in 1964 and his M.D. degree from Marquette University (School of Medicine of Wisconsin, Milwaukee) in 1968. Dr. Poehling’s internship and residency were completed at Duke University Medical Center. He also served in the United States Airforce and it was during his stay in Tachikawa, Japan that he had the opportunity to train under one the first arthroscopists in the world, thus developing his interest in the specialty. He currently is Editor in Chief Emeritus for Arthroscopy, The Journal of Arthroscopic and Related Surgery. In addition to his expertise in arthroscopy, he obtained the Certificate of Added Qualification of Surgery of the Hand by the American Board of Orthopaedic Surgery in 1989. He joined the faculty at Bowman Gray School of Medicine (Wake Forest University Health Sciences) in 1976 and was appointed Chairman of the Department of Orthopaedic Surgery in 1989.
Early in Dr. Poehling’s career, he pioneered the use of arthroscopy to manage orthopaedic pathology of the knee, shoulder, and wrist. Arthroscopy employs a minimally invasive technique to repair cartilage, ligament, and bone pathology within joints allowing patients to recover more quickly after their procedure compared to the open surgical techniques. Since 2007, Dr. Poehling has used unicompartmental knee replacements for patients with knee pain due to osteoarthritis. This technique uses computer-assisted technology and robotics as a less invasive method than total knee joint replacement. He believes that similar techniques can be used to develop computer-assisted technology repair surgery that can be used in combination with arthroscopy techniques. The advantage of the computer-assisted techniques will be that they will support the more accurate placement of ligament repair within the knee, and thus, decrease the incidence of post-operative graft failures. The computer-assisted techniques will shorten the surgical time and result in improved post-operative patient outcomes.
SYNOPSIS OF AREA OF INTEREST: Development of new arthroscopy techniques and surgical instrumentation and the development of minimally invasive surgery with the recent incorporation of tissue engineering.